Inside Your Toolbox: Laser Therapy
Written by Vinh Vuong, PT, DPT
We all have heard of or seen laser therapy one time or another but what exactly is it and how can it affect our treatment strategy? Some may buy into its technique and effects while others may be skeptical. Hopefully this summary will clear up some answers.
History
The idea of laser therapy has been around since the early 1900s when Albert Einstein developed his theory called “Zur Quantum Theories der Strahlung.” It wasn’t until later when the first functioning laser was invented, by Endre Mester, and used on mice to determine whether or not exposure to it caused cancer in 1967. Jumping closer to our present time, the first unit (Class 3B) was FDA approved for the treatment of carpal tunnel syndrome in February 2002. But enough about the history, what is it?!
LASER, Light Amplification by Stimulated Emission of Radiation, is a popular modality that is used throughout the medical field (e.g. dentistry, surgery, physical therapy, acupuncture, etc.). In general, LASER therapy is better termed “Light Therapy” because of the use of different wavelengths being emitted through different diodes from the electromagnetic spectrum. Plus when some people think “laser”, they might think of Star Wars or something that will cause destruction to their tissues. For our purposes in the rehabilitation world, this is not the case. Though there are different types, I think it’s important to understand the basics of low level and high level lasers. [NOTE: keep in mind that discussing the minutiae of laser therapy would require writing a whole book if not more! I only try to focus on the bigger picture that can applied and explained to patients in the clinical setting]
Physiology
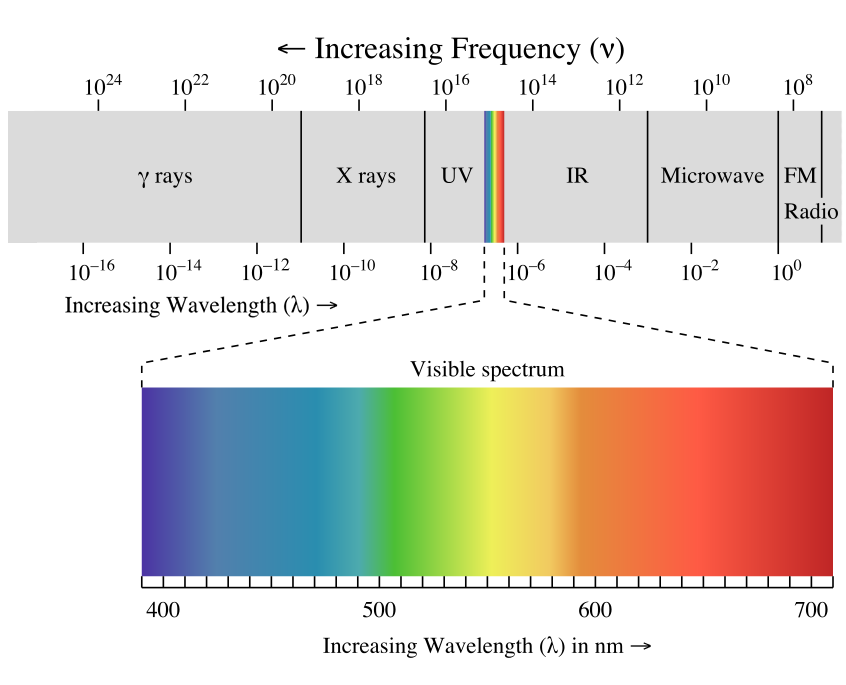
Before diving into the differences, it may be important to understand the physiological aspect of what the light is doing. Whether you have a low-level laser or high-level laser, photons are being released towards the target tissue. These photons are absorbed by the mitochondria and cell membranes, specifically the chromophores (photo-acceptor molecules). The absorbed photons allow for photobiomodulation (defined below) to occur. Depth of the light's penetration depends on the wavelength being emitted, with shorter wavelengths (600nm) being absorbed more superficially and longer wavelengths (904nm) penetrating deeper. One important consideration when deciding the spectrum is the therapeutic window. According to Huang et. al, that window runs approximately from 650nm to 1200nm which almost exclusively involves red and near-infrared light. The term photobiomodulation can be loosely defined as light modifying parts of your biological system and is broken down into photobiostimulation and photobioinhibition. Depending on the dosage, either may occur. When photobiostimulation occurs, there is an increase in the ATP synthesis rate, free nitric oxide (which increases vasodilation), reactive oxygen species (responsible for an anti-inflammatory response), and DNA and RNA production. Photobioinhibition is basically the opposite in that it causes damage to the tissue. In terms of the dosage amount, there is little research indicating the adequate amount.
To break down and compare / contrast the general differences between low-level laser and high-level laser, here’s a table that explains them:
| Low-Level Laser Therapy (LLLT) | High-Level Laser Therapy (HLLT) | |
|---|---|---|
| OSHA Classification | Class IIIB | Class IV |
| Power level | Low power (≤500 mW) | High Power (>500 mW) |
| Method of action | Photobiomodulation | Photothermal or Photobiomodulation |
| Physiological Effect | Enhance cellular function | Cellular destruction or enhance cellular function |
| Usage | Therapy | Surgical or Therapy |
How To Use In A Clinical Setting
According to research, light therapy is effective for treatment of:
- Myofascial/trigger point pain
- Neck & low back pain
- TMJ pain
- Carpal tunnel syndrome
- Dermal wounds
- Tendinopathies
- Rheumatoid/osteoarthritis
- Mixed amount of musculoskeletal pain (eg. Lateral epicondylitis)
The one thing to keep in mind is how you’re using the laser on the patient. When dealing with a low-level laser, you’re less likely to cause tissue damage due to the small amount of power being emitted, whereas the high-level laser can have up to 100x or more power being emitted over the same period of time. With my experience using a class IV laser, it’s important to never stay over one spot for more than a second because of the amount of energy (joules) going into the tissue. The thermal effect given off by the laser, which can be felt by the patient, can be a good indicator of whether it is causing harm to the patient.
When a patient ultimately asks me “what is laser therapy?” I find myself using knowledge gained from my undergraduate degree in Biology to explain it to them. Even though most recommend keeping explanations short and sweet for patients, I personally prefer to get as in-depth as possible, within reason, and stopping just short of when a patient’s eyes begin to glaze over. The way I see it, this demonstrates to them your level of competence in your field of work and increases their confidence in your ability. Basically I explain to them:
“Laser therapy is a type of treatment that uses light to emit energy into your tissues. You see, within your tissues, you have mitochondria – the workhouse of cells in your body that produces a form of energy called ATP. ATP is responsible for regulating cellular processes that allow your body to reach a certain homeostasis. When your tissues become damaged, less ATP is released which causes a delay in healing time. The light from the laser therapy basically stimulates the mitochondria to produce more ATP and allow for healing to occur at a normal rate.”
Summary
To summarize, what is laser therapy? Laser therapy is light being transmitted from a machine to the tissues. There are different devices that have different settings and parameters for its use. There are different types such as low-level lasers which produce less energy (eg. 5 joules per minute) and there are high-level lasers that produce more energy (eg. 20 joules per second). In this write-up, I did not cover or define the specific parameters involved such as power, power density, energy density, dosage per diode, dose tissue, wavelength, irradiance, pulse structure, coherence, or polarization. I wanted to provide an easy summary that will hopefully be useful in a clinical setting if you come across any laser devices. There needs to be more research done to determine adequate dosing amount (time and energy) for different tissues. However, research has shown that laser therapy is an effective modality to use with patients as long as it is administered properly.
Have you ever had experience with using laser therapy on a patient? If so, what were the outcomes for those patients?